Connect With Us

Peripheral Artery Disease and Foot Care

Peripheral artery disease, or PAD, is a vascular condition characterized by the narrowing or blockage of arteries, predominantly in the legs, resulting in reduced blood flow to the feet. This condition, often associated with hardening of the arteries, can significantly impact foot health and lead to various symptoms. Symptoms of peripheral artery disease may include leg pain, cramping, numbness, and skin discoloration. Generally, these symptoms develop when approximately 70 percent of the artery is blocked. Aging, smoking, diabetes, high blood pressure, abnormal cholesterol levels, obesity, physical inactivity, and family history are contributing factors. Men are generally more susceptible to PAD than women. Peripheral artery disease also can result from fibromuscular dysplasia, inflammation, or external pressure from nearby masses. The severity and nature of symptoms depend on the affected artery, degree of blockage, and whether it is a gradual narrowing or sudden blockage. Someone with peripheral artery disease may experience coldness in the lower leg or foot, numbness or weakness, absent or a weak pulse in the legs or feet, and shiny skin on the legs. One of the main dangers is in the formation of sores on the toes, feet, or legs that will not heal. These may develop into ulcers, which can engender severe foot or toe problems. If you have peripheral artery disease symptoms that are affecting your lower limbs and feet, it is suggested that you include a podiatrist as a member of your medical team.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with one of our podiatrists from David A. Scalzo, DPM, PC and Associates. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our offices located in Duryea and Bangor, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral Artery Disease
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
Anatomy of Foot Stress Fractures

Stress fractures are tiny cracks in bones, often seen in the feet due to repetitive stress. Two main types of these fractures exist, consisting of fatigue fractures from overuse and insufficiency fractures in weakened bones. Common in weight-bearing bones like the metatarsals, these fractures result from activities like running and jumping. Symptoms can include localized foot pain and swelling. Diagnosis through imaging is essential. Relief involves rest, reducing impact on the feet, and sometimes using supportive devices, such as crutches or braces. If you have endured a foot stress fracture, it is suggested that you visit a podiatrist who can accurately diagnose and treat this condition.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact one of our podiatrists from David A. Scalzo, DPM, PC and Associates. Our doctors can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our offices located in Duryea and Bangor, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
What Are the Symptoms and Causes of Ingrown Toenails?
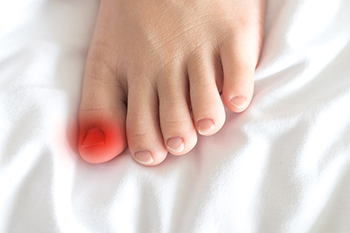
Ingrown toenails, though seemingly minor, can cause significant discomfort and warrant careful attention to both symptoms and causes. One of the primary symptoms is pain, often concentrated along the edges of the toenail, where it begins to grow into the surrounding skin. Swelling and redness may accompany the pain, indicative of inflammation and potential infection. The ingrown nail may also cause tenderness to the touch, making wearing shoes or even walking a painful experience. Causes of ingrown toenails are diverse, often stemming from improper nail trimming, wearing tight or ill-fitting footwear, or inherited structural issues such as unusually curved nails. Trauma or injury to the toe, fungal infections, and poor foot hygiene can also contribute to the development of ingrown toenails. If you have developed an ingrown toenail, it is suggested that you schedule an appointment with a podiatrist who can provide treatment options and effective preventive measures.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact one of our podiatrists of David A. Scalzo, DPM, PC and Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
- Improper toenail trimming
- Genetics
- Improper shoe fitting
- Injury from pedicures or nail picking
- Abnormal gait
- Poor hygiene
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact our offices located in Duryea and Bangor, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ingrown Toenails
Ingrown toenails (onychocryptosis) are a common foot ailment and it is very unpleasant to experience. The condition is caused by an increase in pressure from the ingrowth of the nail edge into the skin of the toe. Ingrown toenails commonly cause pain in those who experience them. In some cases, the skin surrounding the ingrown toenail may break which may lead bacteria to enter through and cause an infection. Common symptoms of this ailment include pain, redness, swelling, and warmth around the toe.
An imbalance between the size of the nail and the enlargement of the nail skin edge causes ingrown toenails. This condition is often caused by improperly trimming the toenails. If you are trying you cut your nails, you should always try to trim straight across instead of in a rounded shape. Ingrown toenails can also be an inherited condition and they may also be caused by improper shoe fitting.
Another common cause of the condition is wearing shoes that are either too small or too large. Other causes include poor foot hygiene, obesity, diabetes, arthritis, edema, and fungal infections. There are many risk factors that may make a person more likely to develop an ingrown toenail. Athletes who play “stop and start” sports such as tennis, soccer, and basketball are most likely to have ingrown toenails.
People who have diabetes, a compromised immune system, or poor circulation should immediately seek care from a podiatrist if they have an ingrown toenail. It is also recommended to seek professional assistance if at-home remedies are not successful within a week or if there is persistent pain.
What is a Sports Podiatrist?
A sports podiatrist is a healthcare specialist focused on treating and preventing foot and lower limb issues in athletes and other active individuals. They have a deep understanding of how the feet and legs function during physical activities and the specific stresses different sports place on these body parts. The role of a sports podiatrist is vital in enhancing athletic performance and preventing injuries. Sports podiatrists conduct thorough assessments, including gait analysis and biomechanical evaluations, to understand an athlete's foot structure and movement patterns. They offer expert advice on appropriate footwear and can design custom orthotic devices to correct biomechanical imbalances, enhance performance, or prevent injuries. They also treat a range of sports-related foot and ankle problems, ranging from overuse injuries to acute traumas. While all podiatrists can treat sports injuries to some degree, a sports podiatrist offers a more focused expertise in managing and preventing injuries specifically in athletes and those engaged in regular physical activities. If you are an athlete and are experiencing foot or ankle problems, it is suggested that you schedule an appointment with a podiatrist who has experience with sports injuries for an evaluation.
If you are dealing with pain in your feet and ankles, you may want to seek help from a podiatrist. Feel free to contact one of our podiatrists from David A. Scalzo, DPM, PC and Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Podiatrist?
A podiatrist is a doctor of podiatric medicine who diagnoses and treats conditions of the foot, ankle, and related structures of the leg. Your podiatrist may specialize in a certain field such as sports medicine, wound care, pediatrics, and diabetic care. Podiatrists have the ability to become board certified through training, clinical experience, and then taking an exam.
What Do Podiatrists Do?
On a daily basis, a podiatrist may perform the following activities:
- Diagnose foot ailments such as ulcers, tumors, fractures, etc.
- Use innovative methods to treat conditions
- Use corrective orthotics, casts, and strappings to correct deformities
- Correct walking patterns and balance
- Provide individual consultations to patients
It is very important that you take care of your feet. It’s easy to take having healthy feet for granted, however foot problems tend to be among the most common health conditions. Podiatrists can help diagnose and treat a variety of feet related conditions, so it is crucial that you visit one if you need assistance.
If you have any questions please feel free to contact our offices located in Duryea and Bangor, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What is a Podiatrist?
A podiatrist is a Doctor of Podiatric Medicine who treats the foot, ankle, and related structures of the leg. If you are having any pain, injuries, or abnormalities in these areas, it is best that you seek help from a podiatrist.
Podiatrists complete four years of training in a podiatric medical school. Their training is like that of other physicians, and they may go on to complete a fellowship training after a residency training. Some podiatrists are board certified meaning they have advanced training, clinical experience, and have taken an exam to prove their skills. Certifying boards for podiatry are the American Board of Foot and Ankle Surgery and the American Board of Podiatric Medicine. Podiatrists may work in private practices, hospitals, clinics, or they may even become professors at colleges of podiatric medicine.
While in college, those who want to be podiatrists often take biology, chemistry, and physics classes in preparation for podiatry school. In podiatry school, students study how the bones, nerves, and muscles work together to help you move around. Additionally, they study injuries and how to properly diagnose and treat them. Admittance into podiatric medical school requires the completion of 90 semester hours of undergraduate study with a good grade point average, and acceptable scores on the MCAT (Medical College Admission Test)
Podiatrists treat many different conditions such as: aching feet, ankle pain, bunions, corns, hammertoes, fungus, ingrown toenails, plantar fasciitis, sprains and more. Common forms of treatment for these conditions are physical therapy, drugs, or surgery. Podiatrists may also recommend corrective shoe inserts, custom-made shoes, plaster casts, and strappings to correct deformities.
Even if you are someone whose feet are in generally good condition, you should still visit a podiatrist to have your feet properly exfoliated and maintained, or to make sure you are looking after your feet properly.
Definition and Underlying Causes of a Bunion
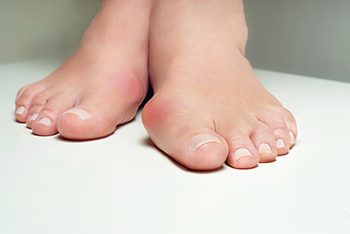
A bunion, or hallux valgus, is a common and often painful foot deformity that affects the joint at the base of the big toe. It manifests as a bony protrusion on the side of the foot, causing the big toe to drift towards the second toe. This misalignment of the joint results in the characteristic bump and can lead to discomfort, inflammation, and difficulty in finding properly fitting footwear. The primary cause of bunions is a combination of genetic and environmental factors. Inherited foot structures that predispose individuals to bunions, like flat feet or low arches, can increase the likelihood of developing this condition. Wearing tight-fitting shoes, particularly those with pointed toes or high heels, can exacerbate the problem or speed up its progression. High levels of stress on the foot or repetitive motion can also contribute to bunion formation. Understanding the causes of bunions is the first step in managing and preventing this condition. When detected early, conservative treatment methods can be helpful. In more severe cases, surgical intervention may be necessary to correct the alignment and provide lasting relief. If you have a bunion, it is suggested that you consult a podiatrist who can guide you toward the most appropriate course of treatment based on your specific condition.
If you are suffering from bunion pain, contact one of our podiatrists of David A. Scalzo, DPM, PC and Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our offices located in Duryea and Bangor, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.